A Guide to Milia: Types, Causes & Treatment Options
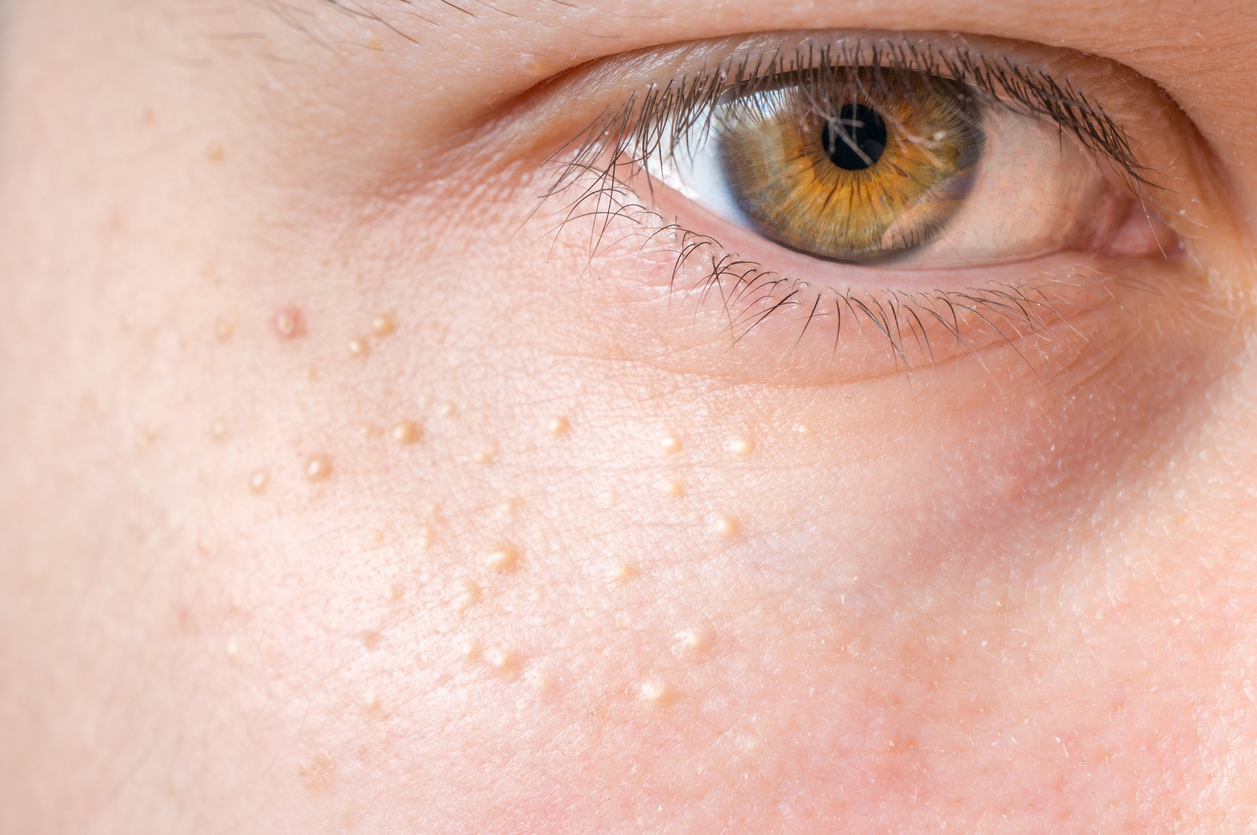
Milia, often referred to as milk spots or oil seeds, are small, benign cysts that appear as white or yellowish bumps on the skin. These cysts are filled with keratin, a protein that is naturally found in skin tissues, hair, and nails. Commonly occurring on the face—particularly on the cheeks, nose, and eyelids—milia can also appear on other parts of the body, including the upper trunk, extremities, and genital area.
These tiny bumps are usually not itchy or painful, but they may cause discomfort for some individuals, especially if irritated by rough fabrics. Although milia are most prevalent in newborns, affecting 40% to 50% of infants, they can occur in individuals of all ages and ethnicities. It is important to note that milia are not a form of acne, though they are sometimes confused with whiteheads due to their similar appearance.
There are two main types of milia: primary and secondary. Primary milia are often congenital, appearing at birth and commonly located on the nose, scalp, and cheeks. Secondary milia, on the other hand, develop in association with skin damage, certain medications, or underlying skin conditions. This distinction is crucial for understanding the various treatment approaches and preventive measures, which will be discussed in subsequent sections of this guide.
What Are The Different Types of Milia?
Neonatal Milia
Neonatal milia are commonly found in infants, presenting as white cysts typically located on or around the nose. These cysts are present at birth and usually resolve on their own within a few weeks. Unlike neonatal acne, milia are of consistent size and lack redness.
Primary Milia
Primary milia appear as small cysts on the eyelids, forehead, cheeks, or genitals. They can occur in individuals of any age, including children and adults. These cysts may disappear naturally over a few weeks but can persist for months if untreated.
Secondary Milia
Secondary milia, also known as traumatic milia, develop after skin damage from burns, rashes, or exposure to sunlight. They may also arise as a reaction to heavy skin creams or ointments. This type typically forms on damaged or inflamed skin areas.
Juvenile Milia
Juvenile milia are cysts linked to inherited conditions and may be present from birth or develop later. These cysts are symptomatic of underlying genetic disorders and require careful diagnosis and management.
Milia en Plaque
Milia en plaque is a rare condition predominantly affecting middle-aged women. It features clusters of milia on an elevated patch of skin, commonly located behind the ears, on the eyelids, cheeks, or jaw. This type tends to form distinct, erythematous plaques that may reach several centimeters in size.
Multiple Eruptive Milia
Multiple eruptive milia involve the sudden appearance of milia groups over weeks to months. These itchy cysts typically form on the face, upper arms, and upper abdomen. While they can occur sporadically, some cases are inherited or associated with genodermatoses.
What Causes Milia
Milia occur when keratin, a protein naturally found in your skin, hair, and nails, becomes trapped beneath the skin’s surface. This usually happens when dead skin cells, which your body typically sheds to make room for new cells, fail to fall away. Instead, these cells get caught under new skin, harden, and form cysts known as milia.
Several factors can contribute to the development of milia:
- Skin Damage: Any form of skin trauma, such as burns, blisters from conditions like poison ivy, or sun damage, can lead to milia as the skin heals.
- Long-term Use of Steroids: Topical or systemic steroids can cause thinning of the skin, making it more prone to trapping keratin.
- Genetic Factors: Some types of milia are linked to genetic conditions, indicating a hereditary component.
- Autoimmune Conditions: In some cases, milia may develop as part of an autoimmune response, where the body mistakenly attacks its own skin cells.
- Lifestyle Factors: Poor skincare habits, using heavy cosmetics that clog pores, lack of sleep, and certain skin conditions like eczema or rosacea can increase your risk of developing milia.
Understanding these causes can help in addressing milia effectively, whether through prevention or treatment.
How to Prevent Milia
While it may not always be possible to prevent milia, especially in newborns, adopting certain skincare practices can help reduce the likelihood of developing milia later in life. Here are some effective strategies:
- Limit Sun Exposure: Protect your skin from excessive sun exposure by wearing sunscreen daily. Choose a sunscreen that is light and non-comedogenic to avoid clogging pores. Remember to apply sunscreen even on cloudy days and during winter months.
- Use Light Moisturizers: Opt for light, non-greasy moisturizers instead of thick creams or ointments which can clog pores and exacerbate milia formation. Moisturizing helps keep the skin hydrated and prevents the buildup of dead skin cells.
- Maintain Clean Skin: Regularly cleanse your skin to remove dirt, oil, and sweat which can contribute to clogged pores. Use a gentle cleanser suited to your skin type and avoid harsh scrubbing which can irritate the skin and lead to more skin issues.
- Exfoliate Regularly: Incorporate gentle exfoliation into your skincare routine 2-3 times a week to help the natural shedding process of dead skin cells, reducing the risk of them trapping keratin beneath the skin.
- Follow Directions on Medications: If you are prescribed steroids or other medications, use them only as directed by your healthcare provider. Long-term or excessive use of steroids can thin the skin, making it more susceptible to milia.
By following these guidelines, you can help keep your skin healthy and potentially reduce the risk of developing milia.
How To Get Rid of Milia
Milia—the small, white bumps that appear when dead skin cells get trapped under the skin—often resolve on their own within a few weeks or months. However, if you find them bothersome, there are several milia removal strategies you can consider.
How to Get Rid of Milia on the Face
For facial milia, you might start with over-the-counter (OTC) exfoliating skincare products. Products containing salicylic acid, glycolic acid, or adapalene (Differin) can help by promoting exfoliation and preventing dead cells from clogging your pores. If OTC products are ineffective, consult a dermatologist for potential treatments like manual extraction, chemical peels, or prescription medications such as topical retinoids.
How to Get Rid of Milia on Eyelids
The skin on your eyelids is extremely delicate, making DIY removal risky. For milia in this sensitive area, it’s best to seek professional help. A dermatologist or an ophthalmologist can safely perform manual extractions or suggest appropriate treatments like laser ablation or cryotherapy, minimizing the risk of damage to your eyes or surrounding skin.
How to Get Rid of Milia Under the Eye
Similar to eyelid milia, those under the eye should be handled with care. Professional extraction by a dermatologist is advised to avoid complications such as scarring or infection. Treatments may include gentle methods like curettage or more advanced techniques such as laser therapy, depending on the severity and persistence of the milia.
How to Get Rid of Milia on Forehead
Milia on the forehead can often be treated with similar methods as those on the face. Begin with gentle OTC exfoliating products. If these are not effective, a dermatologist can perform extractions or prescribe stronger treatments like retinoids. In persistent cases, procedures such as cryotherapy or curettage might be recommended.
Remember, while milia are not harmful, they can be persistent and may require treatment for months. If you’re treating milia at home without success, or if you suspect another condition is causing the bumps, consult a healthcare provider for an accurate diagnosis and appropriate treatment options.
Milia Treatment Options
Milia, while often harmless and self-resolving, can be treated through various methods if their appearance is bothersome. Here are the treatment options you might consider:
For initial treatment, over-the-counter products containing ingredients like salicylic acid, glycolic acid, or adapalene (Differin) can be effective. These products help exfoliate the skin and prevent dead skin cells from clogging pores, which might otherwise lead to milia formation.
If milia persist or if you’re concerned about their appearance, professional dermatological treatments can be more effective. Options include:
- Manual Extraction: Performed by a dermatologist, this procedure involves using a sterile needle or blade to make a small incision and gently extract the contents of the milia.
- Cryotherapy: This method uses extreme cold to freeze and remove milia.
- Laser Ablation: Laser treatments can help remove milia by targeting and vaporizing the cysts.
- Curettage: This involves scraping the skin to remove the milia, sometimes using local anesthesia.
- Chemical Peels: Applying a chemical solution that causes the top layer of skin to peel off, helping to clear the milia.
Prescription Medications
For stubborn or extensive milia, your doctor might prescribe topical retinoids, which are derivatives of vitamin A that help promote cell turnover and prevent the formation of new milia. In cases of milia en plaque, an oral antibiotic like minocycline may be prescribed.
Careful Home Care
For infants, simple daily washing with warm water and mild baby soap can help clear up milia. Adults should maintain a gentle skincare routine, avoiding heavy creams and opting for light, non-comedogenic moisturizers.
It’s crucial to avoid picking or popping milia, as this can lead to scarring or infection. If you’re unsure about the bumps on your skin, consulting a healthcare provider for an accurate diagnosis and appropriate treatment plan is advisable.
Milia Treatment by VitalSkin
If milia are a concern for you, remember to schedule your appointment with a dermatologist for personalized advice and treatment plans. In providing a path toward resolution, we’ve underscored that milia, while common, do not have to be a permanent fixture on your skin. The guidance offered on over-the-counter remedies, professional removal techniques, and the significance of a nurturing skincare routine aims to empower individuals with the knowledge to address milia proactively. The journey toward clearer skin is a testament to the power of informed care and the value of seeking expert advice when necessary. As we conclude, let’s reiterate the importance of a balanced approach to skincare, one that embraces gentle care and seeks professional insight when over-the-counter products fall short, ensuring that your skin remains as healthy and vibrant as possible.
FAQs
What is a milia cyst?
Milia, often referred to as milk spots, are small, white cysts that form under the surface of your skin. These cysts are filled with keratin, a protein naturally found in skin tissues, hair, and nails. They commonly appear on the face but can occur anywhere on the body.
Is milia contagious?
No, milia are not contagious and cannot be spread from person to person. They are simply cysts that form under the skin and are unrelated to any infectious processes.
Does milia go away?
Yes, milia typically resolve on their own. In infants, they often disappear within a few weeks after birth. For adults, milia can persist for a few weeks to several months but usually clear up without the need for medical intervention.
How long does milia last?
The duration milia last can vary. In newborns, milia usually clear up within a few weeks. Adults may notice milia lasting from a few weeks to a couple of months. If you find the appearance of milia bothersome or they do not resolve in a reasonable timeframe, consulting a healthcare provider for potential treatment options is advisable.